Hypothesis / Aims of study
Nocturia, or waking up at night to void, is common and more than 2 voids per night have major impact on health-related quality of life. Nocturia results from an imbalance between bladder storage capacity and urine production. Both inadequate bladder storage capacity that results in small voided volumes and increased urinary output during a 24h period or only overnight (nocturnal polyuria) can be due to various underlying reasons. The International Continence Society (ICS) issued in 2002 a definition of nocturnal polyuria (NP). This was later criticized together with other definitions due to lack of accuracy in identifying nocturnal polyuria 1. Therefore, nocturia remains challenging to manage due to ambiguous definitions of NP and reduced functional bladder capacity (FBC) as well as complexed etiology of this condition. We hypothesized that statistical multivariate modeling may be important and therefore we aimed to determine whether models based on direct factors and indirect factors could accurately predict nocturia in a multivariate analysis.
Study design, materials and methods
The current post-hoc analysis was based on screening data from three prospective phase 3, randomized controlled trials (000085, CS40, CS41) conducted to test the efficacy/safety of desmopressin in 2,575 patients recruited from community and academic practices in Europe and North America. The main inclusion criteria for the screening phase was a complaint of nocturia. Data collection was based on 24 hours frequency volume charts (FVC), collected over three days. Of the 2575 screened patients, we excluded patients with comorbidities such as diabetes mellitus, urological malignancies, uncontrolled hypertension, sleep apnoe, polydipsia, or incontinence (n=391). We also excluded patients with missing FVC (n=670) and finally patients of certain races (n=35) as there were no non-nocturic patients of same race for comparison. Of 1479 included patients, 215 patients were non-nocturic and 1248 were nocturic defined as more than 2 voids per night. Patients had a median age of 59 years (IQR:48-68) with 65% being females. The median number of nocturnal voids was 2.7 (IQR:2.0-3.3)
Factors proposed to influence nocturia were divided into two categories:
Direct factors:
Indirect factors:
We tested:
Results
Interpretation of results
Recognising that mmanagement of nocturia patients are challenging and there is little evidence in reference to the effect of all possible combinations of treatment modalities. The multivariate analysis offered insight in what factors that played a major role. In the multivariate model the indirect factors did not contribute to increasing the predictability, which simplified the model and potentially the diagnosing in terms of information to be collected. The direct factors without a NP definition alone performed worse than when NP definition was included. So the best predictive model includes direct factors including a NP definition. A binary approach to diagnosing nocturnal polyuria may not be optimal if it is recognized that the nocturia is a symptom where several factors contribute. This hypothesis was confirmed by the model. The current binary used definitions of NP were performing worse than the definitions used as a continuum in predicting nocturia. While best predictive models were using NI as definition of NP, this index also captures patients whose nocturia was due to small bladder capacity. Therefore, it was not ideal to describe nocturia caused by an excess of urine production. Instead we suggested to use NUPh which provides almost as good predictive models.
Concluding message
Univariate analyses showed that all NP definitions (continuous and binary) show significant association to nocturic and non nocturic patients. Sleep duration, bladder capacity, sex and race also show significant association.
The correlation analysis showed that the most important correlations appear to be among direct factors of nocturia. Yet, the different definitions of NP only show weak to moderate correlations with each other indicating lack of consistency.
The multivariate analyses showed that the most useful definitions of NP are NI and NUPh. The previously proposed binary NP definitions showed lower predictive performances than when using the continuous indices. These analyses also showed that NI is not a pure definition of NP as it also captures nocturia due to small bladder size. In contrast, NUPh seem to be a good definition of NP alone, leading to good predictive performances when combined to bladder size.
Therefore, we recommend using continuous NUPh as a definition of NP.
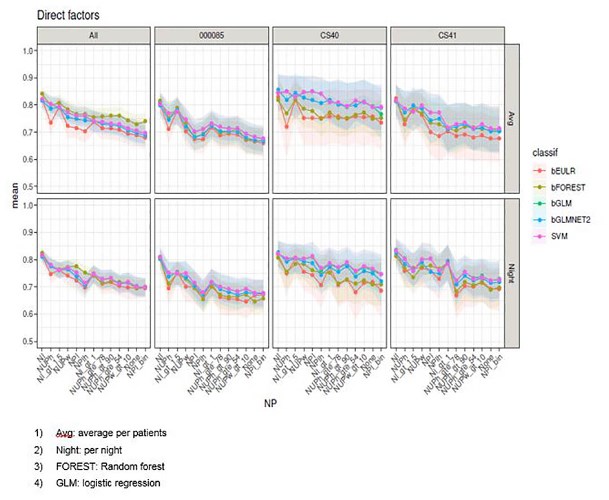
Discriminatory accuracy of different factors in a multivariate combination
References
JL Bosch, K Everaert, JP Weiss, H Hashim, MS Rahnama’i, AS Goessaert et al., 2016: Would a new definition and classification of nocturia and nocturnal polyuria improve our management of patients? ICI-RS 2014. Neurourol Urodyn. 35 (2), 283-287.
Disclosures
Funding Non Clinical Trial No Subjects Human Ethics Committee Central and local Institutional Review Boards in US, Central and local Ethics Committees in Europe Helsinki Yes Informed Consent Yes